Whitney Barron Shares Her Melanoma Journey

Guest blog post by Whitney Barron, Stage 1B Melanoma Thriver:
“When you’re a nurse, you advocate for your patients daily. They put their trust in us to take are of them. So when the roll was reversed, I thought I was being cared for. But unfortunately, I was dismissed, gaslit and told I was being “dramatic” a few times. So for almost three years, while working a very demanding job, I dismissed a mole on my right arm that had been changing. I kept telling myself, maybe it’s nothing, maybe I’m not doing the cream right. Everything but advocating for myself. Not only did it grow and darken, it would itch and bleed. It developed a jagged edge with a darker border. I knew something was wrong, but kept being told it didn’t need a biopsy, didn’t need a dermatology referral and “just keep putting the steroid cream on it.”
I finally made my own dermatology appointment. I know sometimes that is hard to do, but I explained my mole and how long it had been there, and had an appointment shortly after. A biopsy was performed almost instantly. 2 weeks later, on August 28, 2025 I received a text from my doctor, “Hey where are you right now?” We all know what that means, definitely not good. The phone call that followed changed my life forever, I had invassive malignant melanoma, and it was deep. Deep enough that I needed to be referred to a surgical oncologist and preferably a melanoma specialist. My dermatologist was wonderful and knew how long it had been untreated, so she and another nurse practitioner friend got to work getting me the quickest appointment possible.
Telling my husband, children and family I had melanoma was not something I would wish on anyone. At the time my children were 15 and 10 and they did not take it well. It wasn’t a procedure I was going to be able to hide until I knew the biopsy results. It was going to look like a shark took a bite out of my arm. I had to tell them. Then came the question, “mama, are you going to die?” What do you even say to that?! “Well I hope not.” Do you lie? Beause truthfully, I didn’t know if it had spread yet, so my answer would not have been the truth. We did a lot of learning, crying, talking. I notified their schools of what we were going through so they could seek help at school if they needed it. I hope everyone has that kind of relationship with their childrens’ schools, because they were wonderful.

On September 16, 2025, I met with a wonderful doctor at UAB in Birmingham, AL and she had a cancellation on the 19th and could go ahead and do my wide local excision and sentinel lymph node biopsy. She really didn’t want me waiting another month to have my surgery. I was forwarned about the size of my excision, but I don’t think I processed what I was being told. When I woke up in recovery, I cried. I cried when I got home. I cried from the pain. I cried because I knew this big of a procedure could have been prevented. I should have kept pushing, I should have trusted my intuition, I cried because I felt like I didn’t matter to someone I respected and worked for for almost a decade.
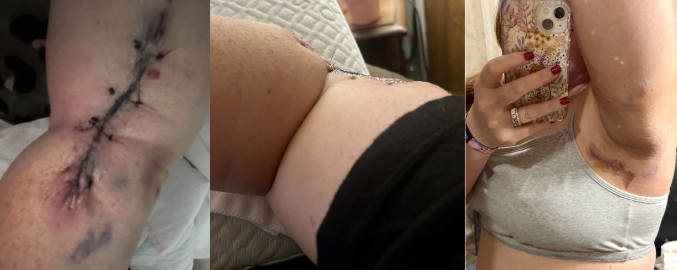
After almost a month, my lymph node biopsy was clear and I was cancer free.
Life after melanoma has been a whirlwind of emotions. I hated my arm and my scar. I have a lot of pain and nerve damage with no feeling at the same time. It’s hard to describe. I have gotten two steroid injections into my scar for keloids, and I see my dermatologist every 3 months for skin checks. I have not had another biopsy since my diagnosis, althought there are spots that we are watching closely.
Another thing I wasn’t truly prepared for, was the toll my mental health would take after my diagnosis. Yes, I’m cancer free, but my mind doesn’t believe that. I feel like I’m constantly having to calm myself down if I think something has changed. You subconsciously feel your lymph nodes. You google things you shouldn’t. You dream about it returning. You lose people you love, whether you’ve met them in person or talk every day via facetime. It is a lot to process. It’s something I struggle with daily.
Even though I’m new to the melanoma world, I jumped into advocacy very quickly. I needed to channel my frustration and emotions into something or I would go insane. I have met the most amazing people. My “melahomies” have been such a blessing through my entire journey. I also was awarded a scholarship to attend Melanoma Research Foundation Advocacy Days in Washington D.C. I had an amazing experience and learned so much. It is intimidating and empowering to lobby for something so personal to you and to people you love.

I’ve had so many opportunitis to spread awareness since my diagnosis. I was invited to throw out the first pitch for the Strike Out Cancer softball game at Troy University, as well as go on to our local radio station to tell my story.
I hope what you take away from my story, is to always advocate for yourself. Get a second and third opinion if you’re not being heard. You deserve a provider or specialist that you trust that will listen to you.
Make sure you’re seeing a board certified dermatologist for your annual skin exams. A quick, 15-20 minute skin exam can save your life. If caught early, melanoma is treatable with higher chances of survival.
-Wear your sunscreen. Whatever kind you like, wear it and reapply it often
Always seek shade when you can
Wear wide brimmed hats and sun protective clothing
Don’t use tanning beds or intentionally lay out in the sun.



